CiTHERA, a new laboratory for the production of therapeutic stem cells
Certified in April 2020, CiTHERA Centre for iPS THERAPIES (Université Paris-Saclay, Inserm, Université d'Évry) is the first production centre for cell therapy derived from pharmaceutical grade pluripotent stem cell engineering. At Genopole (Evry), CiTHERA coordinates the INGESTEM national infrastructure, which is backed by the Models of Malignant and Therapeutics Stem Cells Unit (ONCOSTEM – Université Paris-Saclay, Inserm) in Villejuif. Since August 2020, the centre has been recognised Industrial Integrator by the ‘Plan de relance grand défi’ (Grand Challenge Recovery Plan) to accelerate technology transfer to clinical trials.
Discovered in 1998, human embryonic stem cells (ESCs), obtained from an early-stage embryo, have the capacity to multiply infinitely and are pluripotent, i.e. they can differentiate into any type of cell (blood, nerve, bone, etc.). Their potential for cell therapy is immense as they constitute an almost inexhaustible reservoir for replacing failing cells, whether to regenerate an organ, restore a biological function or eliminate cancerous cells.
In 2006, the Japanese researcher Shinya Yamanaka (Nobel Prize in Medicine in 2012) revolutionised stem cell research. “He showed, first in mice, that it was possible to dispense with the embryo and use reprogrammed adult cells to obtain induced pluripotency cells. Then the following year, he did it using human fibroblasts (skin cells),” explains Director of the CiTHERA Centre, Annelise Bennaceur-Griscelli, who has been working on human ESC since 2004. “This technology was a real turning point.” Like ESCs, induced pluripotency cells (iPSCs) have the capacity to reproduce endlessly and result in all cell types, but do not raise ethical issues related to embryo retrieval.
Modelling pathologies for better treatment
ESCs are used as cell models for the study of incurable genetic diseases, while iPSCs, derived from the reprogramming of any cell type, allow the modelling of all constitutional and somatic genetic diseases such as cancers.
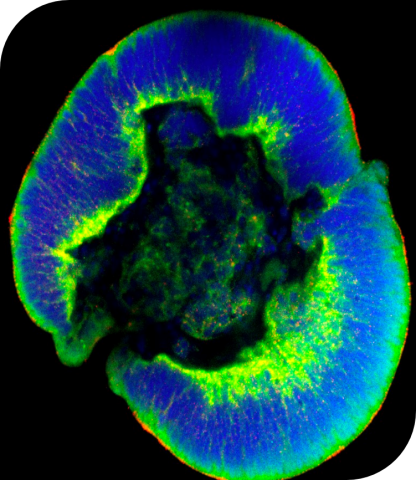
Thanks to a 3D culture technique, these pluripotent stem cells reconstitute complex tissues, called organoids. In the context of cancer, these on-the-chip organs, comparable to mini kidneys, -brains, -lungs... help to elucidate the mechanisms of transformation and progression and to identify new biomarkers and drugs. “Our team is a pioneer in the modelling of hereditary cancers. Somatic mutations in cancers can also be reproduced in these models to study their function and test therapeutic combinations,” Annelise Bennaceur-Griscelli explains.
The rise of basic research
In 2006, “there were already more than 150 embryonic lines available in the United States, whereas in France there were none. The country was lagging far behind,” CiTHERA's director recalls. She brought back ESC lines from the United States to set up the platform, now called ESTeam Paris-Saclay, which derived the first French ESC lines from supernumerary embryos, in collaboration with Professor René Frydman. After S. Yamanaka's discovery, the team immediately began reprogramming. It set up the tools and protocols to derive human iPSC lines by reprogramming blood cells in place of skin fibroblasts. ESTeam then specialises in oncohaematology and cancer modelling to discover new targets.
In 2009, the Models of Malignant and Therapeutics Stem Cells Unit (ONCOSTEM – Université Paris-Saclay, Inserm) was created to open up new fields of research on malignant and therapeutic stem cells. Backed by ESTeam, ONCOSTEM develops 3D organoids derived from iPSCs of various cancers (acute myeloblastic leukaemia, glioblastoma, kidney, lung and breast cancers) and generates CAR (chimeric antigen receptor) cells, i.e. haematopoietic cells (T lymphocytes, NK cells, macrophages) and mesenchymal cells, with a view to cell-based therapies in immuno-oncology or against inflammatory pathologies.
From 2012 to 2020, ESTeam also coordinated the national research infrastructure INGESTEM approved by the ‘Plan investissements d'avenir’ (Future Investments Plan). This platform structures the still emerging research sector by bringing together several French laboratories working on cell reprogramming, differentiation and tissue engineering for pathological modelling and cell and gene therapy.
From research to clinical trials
CiTHERA, the Centre for iPS THERAPIES, is the culmination of a multi-year project to move from research to the production of standardised batches of ESCs and iPSCs and the development of advanced therapy medicinal products (ATMPs).
It is located at Genopole, in Evry, in a 1,500 m² building subject to GMP (Good Manufacturing Practices) and includes three clean rooms for the production of clinical grade iPSC. Genopole – the first biocluster in France entirely dedicated to biotherapies and the development of biotechnology industries – “reflects interest in the project because there is an interesting ecosystem between Université Paris-Saclay and numerous companies and start-ups,” says Annelise Bennaceur-Griscelli.
A well-structured approach
CiTHERA provides the functional link with ONCOSTEM in order to upgrade ESCs and iPSCs from research grade to a raw material for pharmaceutical use. This transfer requires industrial technological solutions for large-scale amplification and qualification of cell batches from a pharmaceutical point of view.
In order to carry out these purposes, the centre is structured in three hubs. An “R&D” hub focused on innovation for the development of CAR therapies, vaccine approaches to cancers and 3D organoids. A “Production” hub focused on the construction of a national bank of clinical grade iPSC cells, and the production of ATMPs from allogeneic and universal cells reducing the risk of immunological rejection. A “Quality” hub responsible for developing international standards, genomic stability and qualitative and functional “potency tests” for therapeutic cell products. Obtaining pharmaceutical accreditation, expected by the end of 2022, is a key step before moving on to phase I/II clinical trials.
Missions and side occupations
CiTHERA also promotes its research through the creation of start-ups. Created in 2018, IPSIRIUS, a spin-out of Inserm and Université Paris-Saclay, for example, received the ILAB award the same year to develop active immunotherapy products from iPSCs and carry out the first clinical trials.
As a member of the steering committee of the project Restore Horizon in charge of unifying and strengthening the development of biotherapies on a European scale, the CiTHERA team is also part of the board of directors of the international consortium Global Alliance for IPS Therapies (GAIT) that is drafting a roadmap of international standards to frame the development of future biotherapies. “We talk a lot in advance with regulatory agencies, such as the EMA (European Medicines Agency) and the FDA (Food and Drug Administration), to help them understand what we do. There is a real sharing of knowledge,” Annelise Bennaceur-Griscelli adds.
In association with the Accelerator for Technological Research in Genomic Therapy (ART-TG - Inserm), CiTHERA, since August 2020 has been a MAGENTA (Manufacturing Cell and Gene Therapy Advances) industrial integrator approved by the Innovation Council as part of the “Biomedicine” major challenge. “The role of integrators is to find technological solutions with start-ups and manufacturers to speed up production and control processes. This partnership opens the way to new synergies in order to find innovative solutions,” Annelise Bennaceur-Griscelli concludes.
References:
- Lucie Portier, Christophe Desterke, Diana Chaker, Noufissa Oudrhiri, Afag Asgarova, Fatima Dkhissi, Ali G. Turhan, Annelise Bennaceur-Griscelli and Frank Griscelli. iPSC-Derived Hereditary Breast Cancer Model Reveals the BRCA1-Deleted Tumor Niche as a New Culprit in Disease Progression. Int. J. Mol. Sci. 2021, 22(3), 1227.
- Desterke C, Griscelli F, Imeri J, Marcoux P, Lemonnier T, Latsis T, Turhan AG, Bennaceur-Griscelli. A. Molecular investigation of adequate sources of mesenchymal stem cells for cell therapy of COVID-19-associated organ failure. Stem Cells Transl Med. 2021 Apr;10(4):568-571.
- Hwang JW, Loisel-Duwattez J, Desterke C, Latsis T, Pagliaro S, Griscelli F, Bennaceur-Griscelli A, Turhan AG. A novel neuronal organoid model mimicking glioblastoma (GBM) features from induced pluripotent stem cells (iPSC). Biochim Biophys Acta Gen Subj. 2020 Apr;1864(4):129540.
- Desterke C, Hugues P, Hwang JW, Bennaceur-Griscelli A, Turhan AG. Embryonic Program Activated during Blast Crisis of Chronic Myelogenous Leukemia (CML) Implicates a TCF7L2 and MYC Cooperative Chromatin Binding. Int J Mol Sci. 2020 Jun 5;21(11):4057.
- Stephen Sullivan, Patrick Ginty, Siofradh McMahon, Michael May, Susan L. Solomon, Andreas Kurtze, Glyn N .Stacey, Annelise Bennaceur Griscelli, Ronald A. Li, Jacqueline Barry, Jihwan Song and Marc L. Turner. The Global Alliance for iPSC Therapies (GAiT). Stem Cell Research. Volume 49, December 2020, 102036.

